Ulcerative Colitis

Comments:
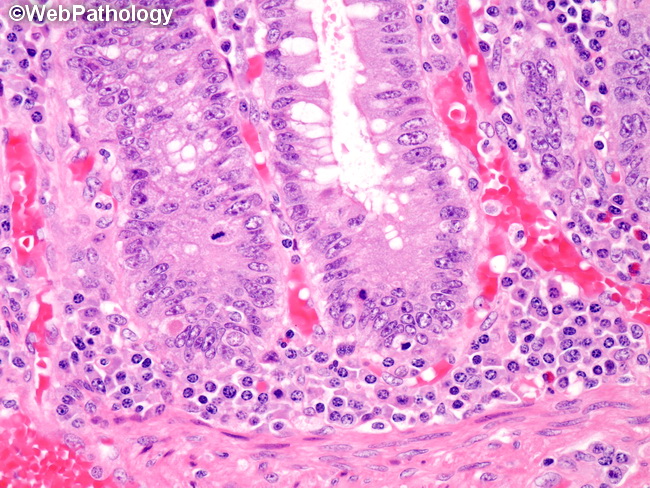
The major histologic changes in ulcerative colitis (UC) are limited to the mucosa and submucosa. There is no transmural inflammation. In the acute stages, there is cryptitis with an increased number of inflammatory cells within the epithelium as well as the lamina propria, including neutrophils, lymphocytes, plasma cells, histiocytes, eosinophils, and mast cells. Basal lymphoplasmacytosis - increased number of lymphocytes and plasma cells between the basal portion of the crypts and muscularis mucosae and one of the hallmark features of UC - is especially well-seen in this image. Granulomas with epithelioid histiocytes and multinucleated giant cells are absent, unlike in Crohn disease. However, mucin granulomas associated with spillage of mucin from ruptured crypts may be present. Numerous lymphoid follicles may be present at the mucosal-submucosal junction. Neutrophils appear in glandular lumen (crypt abscesses) and there is progressive destruction of crypts. Repeated cycles of crypt destruction followed by repair/healing lead to distortion of crypts and decrease in cytoplasmic mucin. Regenerative activity causes reactive atypia in the form of nuclear enlargement and increased mitotic rate. In chronic cases, pyloric gland pseudometaplasia and Paneth cell metaplasia may be seen in distal colon. Normally, Paneth cells are absent beyond right colon.



