Glucagonoma : Clinical Features

Comments:
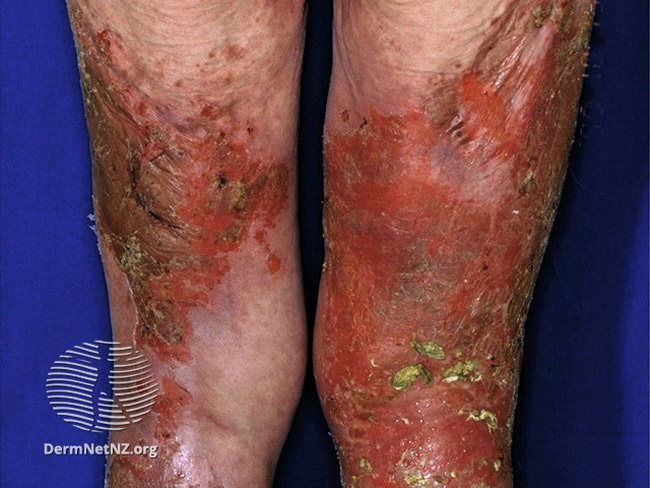
Clinical Features: Glucagonoma usually occurs between 40 and 60 years of age (mean age at diagnosis 52 years). Uncontrolled glucagon synthesis results in glucagonoma syndrome consisting of glucose intolerance (diabetes), anemia, weight loss, depression, deep vein thrombosis, and skin rash (necrolytic migratory erythema, NME). NME is the presenting sign in 70% of patients and may precede the diagnosis of glucagonoma syndrome by several years. The lesions start as erythematous patches in the groin and abdomen and spread to trunk and extremities. The lesions subsequently show superficial central blistering, followed by crusting, healing, and hyperpigmentation. New crops of lesions appear as the older lesions heal. Skin lesions wax and wane and are frequently misdiagnosed (see differential diagnosis). NME is not specific for glucagonoma. Similar skin rashes may be seen in myelodysplastic disorders, hepatitis B, malabsorptive syndromes, cirrhosis, celiac disease, IBD, and other nutritional deficiencies. About 40-60% of patients have oral manifestations (angular stomatitis, cheilitis, and atrophic glossitis; see next image). Diarrhea, neurologic symptoms, and psychiatric symptoms (depression) also occur. Other manifestations include amino acid deficiencies, essential fatty acid deficiencies, normocytic normochromic anemia, and venous thromboembolism (complicated by pulmonary embolism in some cases). About 50-70% of patients have liver metastases at initial presentation. Other metastatic sites include regional lymph nodes, mesentery/peritoneum, spleen, bones and lungs. Patients with glucagon cell hyperplasia and neoplasia do not have full-blown glucagonoma syndrome but present with abdominal discomfort along with elevated glucagon levels (10-20 times normal).Image source: Dermnet NZ; used under license: Creative Commons Attribution-NonCommercial-NoDerivs 3.0 (New Zealand).



