Ulcerative Colitis : Pathogenesis-II

Comments:
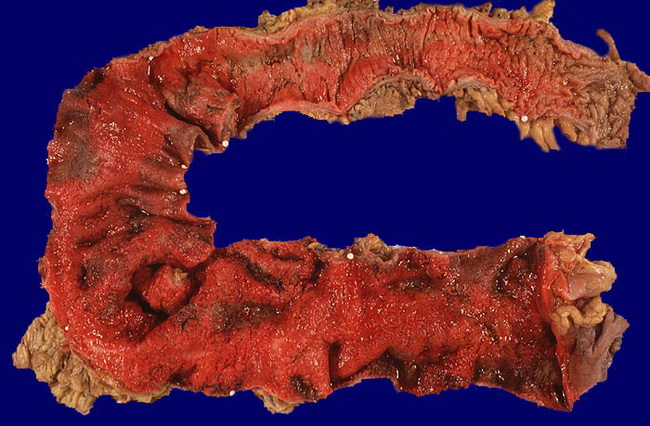
The etiology of inflammatory bowel disease is unknown; however, there appears to be a complex interplay of genetic susceptibility, host immunity, and environmental factors. Several pathways are involved, including: MUCOSAL IMMUNE RESPONSES: Inappropriate mucosal immune responses to gut bacteria are considered to play a key role in the pathogenesis of IBD. T helper cells (TH1 and TH17) are activated in Crohn disease. Certain polymorphisms of IL-23 receptor which regulates TH17 cells reduce the risk for both Crohn disease and UC. Inflammatory cytokines such as TNF, interferon-� and IL-13 are involved in the pathogenesis of IBD. Autosomal recessive mutations of IL-10 and its receptor are linked to severe, early onset IBD. Given the central role played by defective immune responses in the development of Crohn disease and UC, immunosuppressive agents are a key component of therapeutic regimens. EPITHELIAL DEFECTS: A number of epithelial defects have been found in Crohn disease and UC, including defective barrier function of intestinal epithelial tight junction. This defect is associated with specific NOD polymorphisms. In addition, UC is associated with polymorphisms involving ECM1 (extracellular matrix protein 1) and transcription factor HNFA. ROLE OF INTESTINAL MICROBIOTA:: The concentration of intestinal bacterial is quite high in the colon. The patients whose Crohn disease is associated with NOD2 variants show antibodies against bacterial protein flagellin. Anti-flagellin antibodies are uncommon in UC. Clinical trials have shown beneficial effects of probiotic bacteria and fecal microbial transplants from healthy individuals. According to one model of IBD pathogenesis, defective barrier function at intestinal epithelial tight junctions allows bacterial components to access lamina propria and activate innate and adaptive immune responses. The release of TNF and other cytokines increases tight junction permeability which allows even greater amount of bacterial components. This sets up repeated cycles of cytokine-induced mucosal damage, inflammation and ulceration followed by regeneration and healing. The image shows fulminant ulcerative colitis in a 47 y/o female who underwent emergency colectomy. The mucosa is inflamed and appears granular. Note the loss of normal mucosal folds. Image copyright: pathorama.ch



